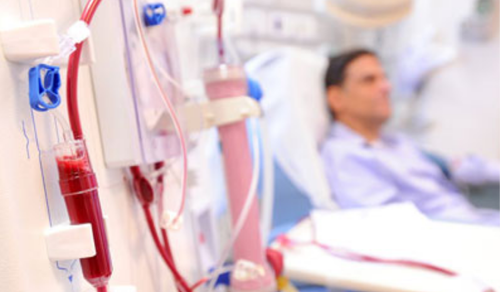
In a new research, it is found that adults on dialysis having employer-sponsored plans that have shifted to Medicare have faced less financial risk than before. If the patients drop their End-stage Kidney Disease(ESKD) due to lay-off, and disappointment with the plan, then Medicare becomes their primary payer and they face a reduced monetary burden upon their shoulders.
- According to a study published in JAMA Network Open, one-third of the adults who began dialysis with an employer-based group health plan rearranged to Medicare before the due date, resulting in $3 billion additional Medicare costs over ten years.
- In this following study, researchers analyzed the US Renal Data System for 113,693 adults ages 62 years or younger who started dialysis between 2007 and 2014. The study found that overall 33% of the patients switched from employer-sponsored health plans to Medicare prematurely contributing to 711,528 additional months of Medicare coverage which resulted in $81,000 of Medicare cost per participant.
- An Alliance of Community Health Plans fact sheet from January 2021 noted, “ Congress created Medicare Advantage(MA) in 2003 to provide America’s seniors a convenient, coordinated opinion for their health coverage and to drive greater value and accountability in the Medicare program”.
- The researchers called for policy interference that would lead to sharing financial risk among Medicare and EGHP. One of the writers wrote, “ frequent premature switches to Medicare likely discourage EGHPs from Funding cost-saving intervention that prevents ESKD in chronic kidney disease because switching to Medicare prematurely offloads more than $80,000 of financial risk per patient”.

